Case Studies
Case 1 : Successful Surgical Management of WHO Grade II Atypical Meningioma with Mesh Cranioplasty
Introduction
Meningiomas are among the most common primary brain tumors. While many are benign, atypical (WHO Grade II) meningiomas carry a higher risk of recurrence and require timely surgical management and structured follow-up.
This case highlights the successful treatment of a symptomatic frontotemporal meningioma with gross total excision and immediate mesh cranioplasty, resulting in excellent neurological recovery and seizure control.
Patient Profile
Age/Gender: 45-year-old male
Presenting Complaints:
Progressive headache
Recurrent seizures
The patient presented with worsening headaches over several months along with new-onset seizure episodes. Given the neurological symptoms, urgent brain imaging was advised.
Diagnostic Evaluation
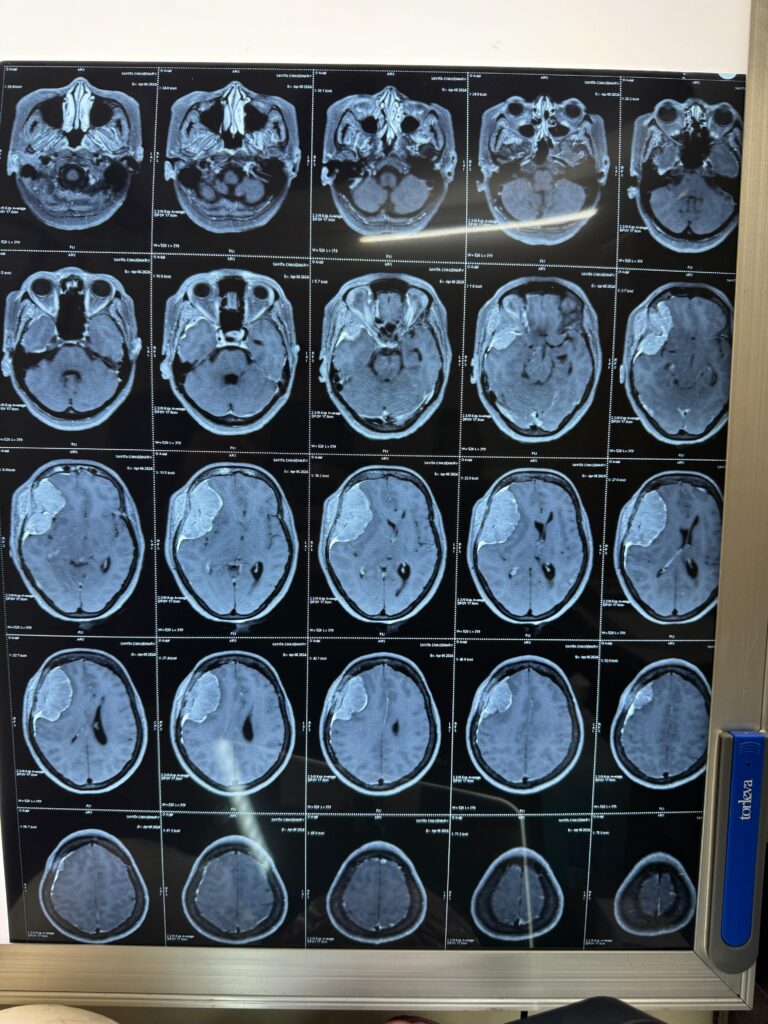
Magnetic Resonance Imaging (MRI) revealed:
Location: Right frontotemporal region
Lesion Type: Extra-axial mass
Radiological Impression: Suggestive of meningioma
Mass Effect: Significant compression of adjacent brain tissue
The imaging findings indicated a space-occupying lesion causing symptomatic mass effect, necessitating surgical intervention.
Surgical Procedure
The patient underwent a single-stage surgical procedure.
Approach: Right frontotemporal craniectomy
Tumor Resection: Gross total excision achieved
Intraoperative Findings:
Well-defined tumor margins
Moderately vascular lesion
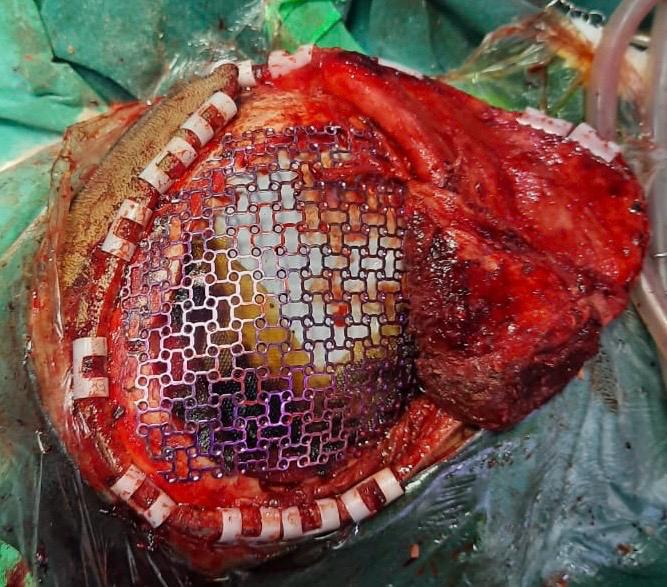
Reconstruction: Immediate mesh plate cranioplasty performed in the same sitting
The tumor was completely removed without intraoperative complications, and cranial reconstruction was carried out using a mesh plate to restore skull integrity and contour.
Histopathological Diagnosis
Microscopic examination confirmed:
Diagnosis: Meningioma
WHO Grade: II (Atypical)
WHO Grade II meningiomas are associated with an increased risk of recurrence compared to Grade I tumors, making complete excision and regular follow-up essential.
Postoperative Outcome
Uneventful postoperative recovery
Significant improvement in headache
Effective seizure control
No new neurological deficits
Good functional recovery
The patient was discharged in stable condition and advised routine follow-up with serial imaging.
Conclusion
Timely surgical intervention with complete tumor excision remains the cornerstone of management for WHO Grade II atypical meningiomas. Combined with immediate mesh cranioplasty and structured postoperative follow-up, patients can achieve excellent functional outcomes and quality of life.
Regular clinical and radiological surveillance is essential to monitor for recurrence.
